GALLSTONES DISEASE: Causes, Risk Factors, Symptoms, and Treatment
Welcome to our guide on gallstones disease. Explore the causes, risk factors, symptoms, treatment options, risk factors for surgery and recovery process with this condition.
Causes of gallstones?
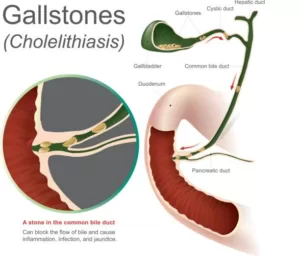
Gallstones form due to an imbalance in the substances present in bile, a digestive fluid produced by the liver. The main types of gallstones are:
- Cholesterol Stones: Excess cholesterol in the bile leads to the formation of the most common type of gallstones. Cholesterol stones vary in size and color.
- Pigment Stones: Less common, these stones are composed of bilirubin, a pigment produced during the break down of red blood cells. Pigment stones are smaller and darker in color.
- Mixed stones: Two or more substances, including cystine, calcium, phosphate, and protein, form these types of gallstones.
Are there risk factors for gallstones disease?
Certain factors increase the risk of developing gallstones, such as:
- Gender: Women, due to higher estrogen levels, are more susceptible to gallstones formation.
- Hormone replacement: Taking hormone replacement therapy or birth control may increase risk.
- Age: The risk of gallstones increases with age, (after 40 years old).
- Obesity: Being over-weight raises the risk of gallstone formation.
- Family history: Having a family history of gallstones increases the likelihood.
- Diet: A diet high in cholesterol and fat but low in fiber increases the risk.
- Rapid weight loss: Losing weight too quickly can trigger gallstone formation.
What are the common symptoms of gallstones disease?
Gallstones are very common in the general population, affecting about 10-15%. Fortunately, 80-90% of cases are well without any symptoms and do not require any treatment.
Gallstones may cause sometimes cause the following symptoms:
- Tummy pain: Severe pain in the upper abdomen that can radiate to the back or shoulder.
- Nausea and vomiting: Feeling nauseous and vomits.
- Jaundice: Yellowing of the skin and eyes if gallstones causing blockage of bile ducts.
- Indigestion: Difficult to digest fatty foods, resulting in bloating, gas or heartburn.
- Fever and chills: Infection of the gallbladder can cause fever and chills.
What are the complications from gallstones disease?
Gallstone disease can lead to several complications, including:
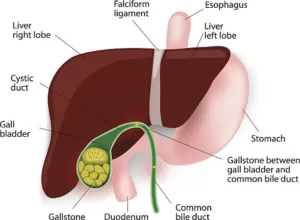
Cholecystitis: This is infection or inflammation of the gallbladder that occurs when a gallstone blocks the cystic duct. Thus, it can cause severe pain in the upper right abdomen, fever, and nausea.
Choledocholithiasis: If a gallstone passes from the gallbladder into the common bile duct, it can block the flow of bile into the intestine. This condition can cause jaundice, abdominal pain, and potentially lead to infections such as cholangitis or pancreatitis.
Gallstone Pancreatitis: If a gallstone obstructs the pancreatic duct, it can cause inflammation of the pancreas. This condition is known as gallstone pancreatitis and can result in severe abdominal pain and potentially life-threatening complications.
Cholangitis: This is an infection of the bile ducts that occurs when a gallstone blocks the bile flow. It can cause symptoms such as fever, jaundice, abdominal pain, and can be a medical emergency.
How to diagnose gallstones disease?
These are example of common test for diagnosing gallstones:
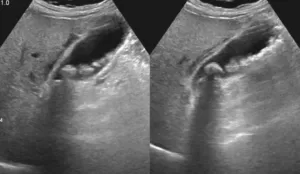
- Ultrasound: This imaging test is most commonly used to identify the presence of gallstones.
- Blood Tests: Doctor may conduct blood tests to check for high levels of bilirubin or liver function abnormalities.
- CT Scan or MRI: These imaging tests may be used to get a detailed view of the gallbladder and surrounding structures.
What are the treatment options gallstones disease?
The treatment approach for gallstones depends on the severity of symptoms and complications. The following options are available:
- Conservative: If gallstones are asymptomatic, your doctor may recommend monitoring without any surgery. This scenario is most common when gallstones are incidental findings from imaging performed for other purposes
- Laparoscopic Cholecystectomy: The most common surgical procedure for gallstones, involving minimally invasive (keyhole) removal of the gallbladder through a few small incisions.
- Open Cholecystectomy: In complex cases, an open cholecystectomy may be necessary, involving a larger incision for gallbladder removal.
More on Laparoscopic Cholecystectomy
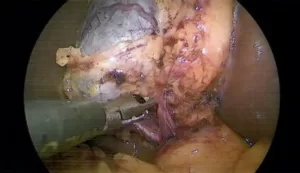
Laparoscopic (keyhole) cholecystectomy is a minimally invasive surgical procedure performed to remove the gallbladder.
- The surgery is performed under general anesthesia.
- Several small incisions are made in the upper abdomen.
- A laparoscope, which is a thin, flexible tube with a camera and light source, is used to visualize the surgical field.
- The surgeon inserts surgical instruments through the other incisions to remove the gallbladder.
What are the potential complications of Laparoscopic Cholecystectomy?
Some potential risks of the surgery including:
- Infection: Infection at the surgical site or in the abdomen.
- Bile Duct Injury: Damage to the bile ducts during surgery.
- Bleeding: Liver bed injury may lead to significant bleeding.
- Digestive Problems: Changes in digestion, such as diarrhea or difficulty digesting fatty foods.
What are the recovery process after Cholecystectomy Surgery?
Here are some key aspects of the recovery process:
- Hospital Stay: Surgeons typically discharges most patients on the same day after laparoscopic cholecystectomy. Open cholecystectomy may necessitate a longer hospital stay.
- Pain Control: Pain is common during first week after surgery and adequate analgesia will be given.
- Dietary Changes: Your surgeon may advise you to follow a special diet initially and slowly return back to regular food.
- Physical Activity: Light activities can be resumed soon after surgery, but more strenuous activities should be avoided for 8-12 weeks.
Other General Surgery
- Appendicitis
- Skin Lesions
- Abscess
Consult us

Dr LEE Kuok Chung
Senior Consultant General Surgeon
Subspeciality interest: Colorectal, Advanced Endoscopy and Robotic Surgery

Dr TAN Wee Boon
Senior Consultant General Surgeon
Subspeciality interest: Thyroid, Hernia and Endocrine Surgery

Dr KIM Guowei
Senior Consultant General Surgeon
Subspeciality interest: Upper Gastrointestinal, Bariatric and Robotic Surgery
Crest Surgical Practice
Healing Hands, Compassionate Hearts: Your Partner in Surgical Care

