Thyroid Cancer Surgery
Understanding Thyroid Cancer Surgery: Procedure, Recovery, and Risks
How is thyroid cancer treated?
 There are many sub-types of thyroid cancer. Papillary and follicular thyroid cancers account for 80-90% of them. They tend to grow slowly and if detected early, both can be treated successfully.
There are many sub-types of thyroid cancer. Papillary and follicular thyroid cancers account for 80-90% of them. They tend to grow slowly and if detected early, both can be treated successfully.
Thyroid cancer surgery remains the main treatment in most cases of thyroid cancer.
 There are many sub-types of thyroid cancer. Papillary and follicular thyroid cancers account for 80-90% of them. They tend to grow slowly and if detected early, both can be treated successfully.
There are many sub-types of thyroid cancer. Papillary and follicular thyroid cancers account for 80-90% of them. They tend to grow slowly and if detected early, both can be treated successfully.
Thyroid cancer surgery remains the main treatment in most cases of thyroid cancer.
How is thyroid cancer surgery performed?
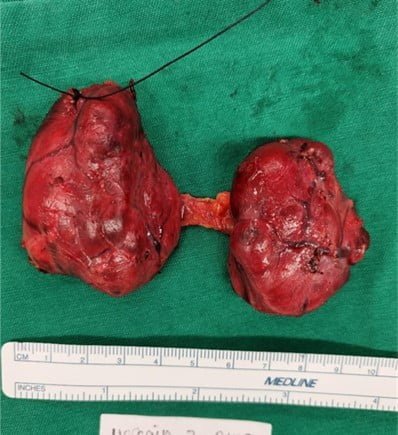
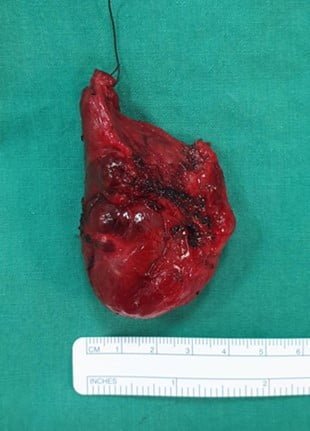
Thyroidectomy refers to the surgical removal of the thyroid gland. This can be total thyroidectomy where the entire thyroid gland is removed, or hemithyroidectomy where only the diseased side is excised. Your surgeon will recommend which is the most appropriate surgery of choice for your case.
Nodulectomy refers to the excision of the nodule of concern and it is no longer considered appropriate in both benign and malignant cases.
The surgery is performed under general anaesthesia and the patient will normally stay overnight after the procedure. A small incision is made over the lower part of the neck. This runs in the same direction as the natural crease of the skin thus minimizing pain and scarring. The thyroid gland is then reached after dividing the superficial fat and muscle layers. The thyroid is then removed completely after division of its blood supply and identification and preservation of the recurrent laryngeal nerve. The wound is then closed in layers with the absorbable skin sutures underneath the wound.
Most patients will be discharged in 1 to 2 days. You may have to stay a few days longer for intravenous calcium replacement if your calcium level is low.
What is the incision for thyroid surgery?

Thyroidectomy is most commonly performed via an open method through the neck. In selected cases, it be done via incisions away from the neck such as through the armpits and/or nipples or through the mouth.
How is the healing process?
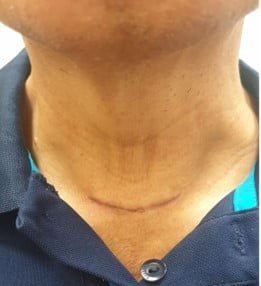
The skin crease incision in the neck is about 4-6cm. The is a small risk of wound infection (<1%) during first week after surgery. As absorbable sutures are used, there is no need to remove any sutures after surgery. Wound will appear to be red initially but will gradually fade away after a few months.
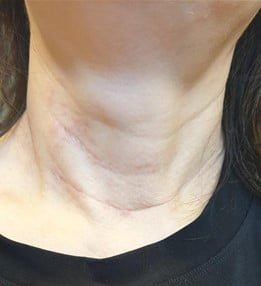
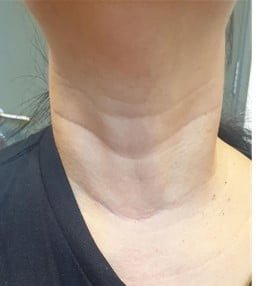
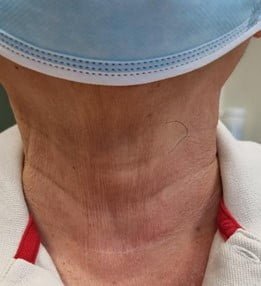
Scars once fully healed will look similar to natural skin creases
What are the risks involved?
Thyroid cancer surgery is almost never life threatening and the rate of complications is extremely low when performed by experienced thyroid surgeons. The risks involved in any surgery such as bleeding and wound infection can also occur in thyroid cancer surgery. Most patients find the wound pain manageable and do not require any painkillers after 3 to 5 days. The risk particular to thyroid cancer surgery is recurrent laryngeal nerve palsy with resultant hoarseness of voice that occurs in less than 2% of the time. Majority of these are temporary and will recover with time.
In cases of total thyroidectomy where the entire thyroid gland is removed, patient will need lifelong thyroxine supplements after the surgery. There are no side effects from the medications as thyroxine hormones are essential to our body’s metabolism. Some patients might need calcium and vitamin D supplements as well after surgery.
What is the follow up after discharge?
Your surgeon will see you in 1 to 2 weeks to review the wound and the histology report. You will need blood tests in a few weeks after surgery to monitor the thyroid hormone and calcium level. Depending on the final histology report, you may be advised for further treatment with radioactive iodine therapy (RAI) in 6 to 8 weeks after surgery. A nuclear medicine specialist will explain and arrange the RAI treatment for you.
Subsequent follow ups will involve clinic visits with blood tests and thyroid ultrasound to monitor for disease recurrence.
Book Appointment
Book your consultation today for expert surgical care.
